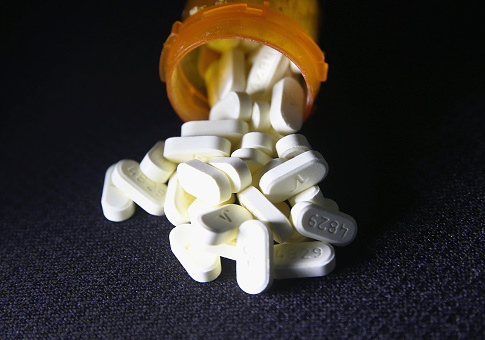
Children in a cohort of Tennessee Medicaid enrollees "frequently" received opioid prescriptions for non-chronic diseases, a new study from researchers at Vanderbilt University concluded.
The study found that an average of 15 percent of children were prescribed opioids for acute conditions, a figure that rose steadily from 1999 to 2003, plateaued, and then fell starting in 2009.
More than 40,000 people died from opioid overdoses in 2016, a number that is likely to have increased less quickly but not fallen in 2017. Nationwide, drug overdose death is the number one cause of injury death, outpacing homicide, suicide, and car crashes thanks largely to opioid overdoses.![]()
However, less is known about the approximately quarter of the country under the age of 18. Data are available on treatment of adolescents for opioid overdose and poisoning, both of which have risen over the past several decades. These data only cover cases of children already hospitalized or exposed to the medical establishment, therefore telling us little about the number of opioids kids are consuming "in the wild" as it were.
To fill this gap, the study's authors examined data from Tennessee's Medicaid program between 1999 and 2014. They specifically omitted children with severe, chronic conditions—like cancer or sickle cell anemia—to try to understand how frequently kids were being prescribed opioids for acute, routine illnesses.
As previously mentioned, they found that among this group, an average of 15 percent of the child enrollees were prescribed opioids over the course of the study. Kids age 12 to 17 were the most frequent recipients of opioid prescriptions, with between 15.8 and 26 percent of that group prescribed opioids depending on the year.
![]()
These prescriptions were most frequently for dental procedures (31.1%), followed by outpatient surgical or medical procedures (25.1%), trauma (18.1%), and minor infections (16.5%). The median opioid dose was 0.5 to 0.6 milligrams per kilogram of child's weight per day. The most commonly prescribed drug was hydrocodone (aka Vicodin), followed by codeine; the two drugs together accounted for more than 80 percent of prescriptions.
The study also estimated the number of opioid-related adverse events, including ER visits, hospitalizations, and deaths: three over the course of the study. Cumulatively, the study's authors estimated that there were about 38.3 opioid-related adverse events per 100,000 prescriptions, with the most common symptoms being gastrointestinal, neuropsychiatric, dermatological, and depression of the central nervous system.
All of this suggests that the use of opioids among children is more common than one might expect. The incidence rate of opioid-related adverse events, especially deaths, is quite low. However, it is worth noting that few opioid overdose deaths are attributable to opioids an individual has been directly prescribed (as opposed to diverted for abuse purposes).
Further, the number of opioid prescriptions among children has already peaked, at least assuming the data from Tennessee generalize to the adult population. This mirrors the trend in the general population, with the prescribing rate falling continuously since 2012.
"Nevertheless," the study's authors conclude, "the prevalence of opioid prescriptions for children in the study remained >10% by 2014. The frequent prescribing of opioids in this population, including codeine, which now is considered a suboptimal analgesic choice for children, underscores the need for education regarding multimodal opioid-sparing regiments."