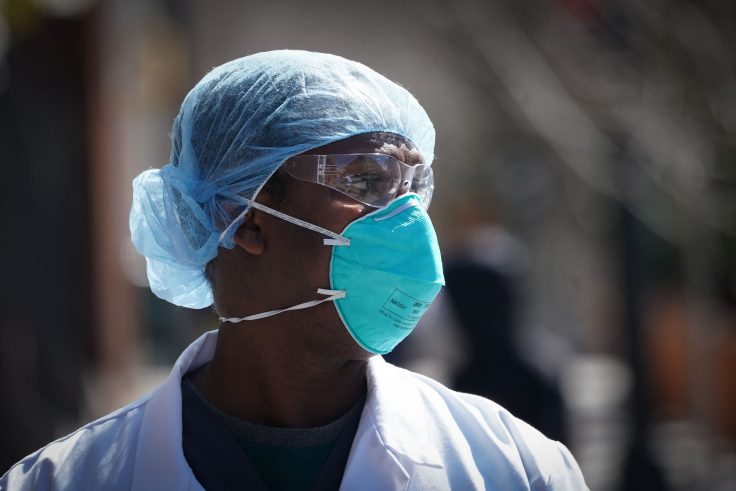
As medical professionals fighting the coronavirus face a dangerous shortage of special protective masks, a group of engineers and entrepreneurs are trying to make such masks in the United States—but face major obstacles.
The Open PPE Project is trying to ensure availability of N95 respirators, which are in short supply as the coronavirus besets the United States, by creating an American supply chain that would ensure the country can manufacture them in a global crisis, now or in the future.
The group's efforts have run up against serious regulatory barriers, however, as a federal bureaucracy struggling amid the epidemic lacks the resources to bring such a project online. One of the project's leads, Matt Parlmer, told the Washington Free Beacon that his project cannot even begin, as federal inspectors remain under-resourced and stuck at home under a federal ban on nonessential travel.
The barriers faced by the Open PPE Project and other nontraditional manufacturers looking to combat the pandemic offer a prime example of regulation standing in the way of a swift response to COVID-19. They also represent an opportunity for the White House, which has demonstrated a willingness to cut red tape aggressively.
Parlmer and the rest of the Open PPE team have been working since early March. They aim to domestically manufacture a variety of personal protective equipment, but will start with N95 respirators, which filter out very small particles and are widely used in hospitals throughout the country. The United States currently has just 10 percent of the masks the Department of Health and Human Services projects it will need. In New York state, currently the center of the coronavirus outbreak, medical professionals are going without these life-saving masks, leading to dangerous, even deadly, infections.
Almost from the beginning, however, Open PPE has run up against regulatory barriers. The National Institute for Occupational Health and Safety (NIOSH)—the subdivision of the CDC responsible for ensuring quality standards for N95 respirators—told the Open PPE Project that approval could take one-and-a-half to three months, a lifetime in pandemic terms.
In order to get production off the ground, Parlmer explained, NIOSH would need to certify that the masks his group produced are able to form a tight seal on the wearer's face and adequately filter particles. An examination by the National Personal Protective Technology Laboratory (NPPTL)—the sub-branch of NIOSH responsible for conducting such tests—would take time and energy the pandemic-slammed agency simply does not have.
This situation is complicated by the travel restrictions imposed on federal employees in mid-March limiting all but "mission-critical" travel. Running an N95 manufacturing facility would require an NPPTL official to conduct site inspection, which is impossible if he or she cannot travel. The CDC did not respond to a request for comment as to whether NIOSH employees have been exempted from the restrictions, but Parlmer was doubtful.
"If site examinations are a part of this process, and people can't leave the town that they live and work in, we're sort of at a standstill with this thing," Parlmer said.
The CDC told the Free Beacon that the NPPTL is currently focused on supporting existing manufacturers, evaluating new respirator applications for approval, and providing "up-to-date PPE guidance." It was not able, according to a public affairs officer, "to provide consultation concerning new respirator manufacturing approaches, or assistance to non-traditional manufacturers who are interested in switching operations to respirator manufacturing."
This is not, Parlmer said, for lack of trying. Behind the scenes, the NIOSH officials to whom he and his team have spoken are frustrated that they cannot help.
"They want to be able to get out of the way, too," he said. "The test engineers involved here, these are good guys, they're just trying to keep people safe."
Open PPE's is not the first case of a regulator slowing down life-saving development. As the disease raged in other countries, regulatory barriers imposed by the CDC and FDA set widespread coronavirus testing in the United States back by months. In a recent editorial, former FDA chief Dr. Scott Gottlieb argued that regulators would need to be incredibly careful in order to not slow the development of life-saving antiviral treatments.
The best fix for his problem, Parlmer argued, would be for NIOSH to call for back-up, granting high-quality university laboratories temporary authority to conduct quality testing. This would substantially expand the number of experts able to approve N95 production and obviate the need for NPPTL officials to travel to conduct site inspections.
"If we could get some sort of executive directive, something from the White House directing NIOSH to delegate approval to qualified university laboratories, that alone would be huge," Parlmer said. "We'd rather it go wider than that to anybody who can validate the equipment, but we'd be willing to settle for just university laboratories, as that would multiply the amount of available certification equipment several times."