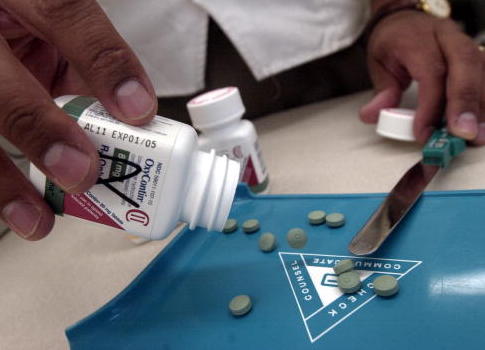
A new study casts doubt on the efficacy of popular programs meant to curb prescription opioid overdoses.
Deaths associated with prescription opioid abuse have risen steadily since the late 1990s, driven by a wave of prescription pills pushed by pharmaceutical firms and dispensed by doctors. Central to propagating the crisis are already-hooked patients, who might approach a doctor claiming some unspecified malady just to score drugs.
Prescription Drug Monitoring Programs (PDMPs) are electronic tools for keeping track of which doctors have prescribed which pills to which patients, and when. They allow doctors to know, for example, when a patient has visited too many doctors looking for pills; they also allow states to track which doctors might be too generous with their prescription pads. The idea is popular: 49 of 50 states have set up a PDMP.
However, "there is a paucity of data on the effects" of PDMPs, the study's authors note. Do the programs actually cut the number of opioid prescriptions? Do they block anyone who would have gotten an opioid prescription otherwise?
To answer this question, the authors performed a study at the hospital where they worked, the Dartmouth-Hitchcock Medical Center in Lebanon, N.H. On Jan. 1, 2017, New Hampshire launched its PDMP, creating a natural disjuncture which the study takes advantage of to assess trends in opioid prescribing practices.
The results are less than stellar for the PDMP. The percentage of patients prescribed opioids after surgery did not change significantly in the six months before and after Jan. 1. Additionally, the average number of pills prescribed to a patient fell far more in the six months before the PDMP was set up than in the six months after—a 22 percent decrease vs. a 3 percent decrease.
What is more, the study's authors identified no cases where a query to the PDMP resulted in a patient actually being denied opioids.
"The intended effect of the PDMP query and risk calculator to avoid opioid prescriptions likely to be abused or diverted was not supported in our study," the authors conclude.
Importantly, the study's scope is restricted only to patients who are being prescribed opioids after surgeries. As the authors note, "while some patients may feign back pain in an attempt to obtain an opioid prescription in a walk-in clinic, it is highly unlikely that they will undergo a surgical procedure just to obtain opioids." And another study, cited by the authors, indicate that PDMPs have been more successful in clamping down on scams at non-surgical pain clinics.
However, that does not mean that there are no implications to the study. PDMP checks are viewed by some doctors as inconvenient and onerous, and the study indicates that at least for surgeons, that time may be better spent doing something else.
More significantly, the study indicates an area where PDMPs are insufficient to combat prescription opioid overdoses. That is because most instances of addiction and death aren’t attributable to directly prescribed pills, but rather to prescribed pills sold, stolen, or otherwise diverted for misuse. If a surgical patient does not use his whole prescription, then he leaves drugs ripe for abuse, an issue with which surgeons remain ill-equipped to deal.
"The more unused painkillers or controlled drugs we can help to remove from homes, the more potential lives will be saved. The home medicine cabinet is a frequent target of prescription drug abusers and often provides access to prescription medication," said former Acting Drug Enforcement Agency Administrator Robert W. Patterson in April.